Como cada 12 de mayo, se celebra el Día Europeo de la Periodoncia. La conmemoración de esta fecha está promovida por la European Federation of Periodontology (EFP) e impulsada en España por la Sepa (Sociedad Española de Periodoncia y Osteointegración). Como especialistas en periodoncia e implantes, nos sumamos a las iniciativas de divulgación y concienciación sobre las enfermedades periodontales. Aprovechamos, por lo tanto, para desgranar el “abc” de las enfermedades periodontales.
¿Qué es el periodonto?

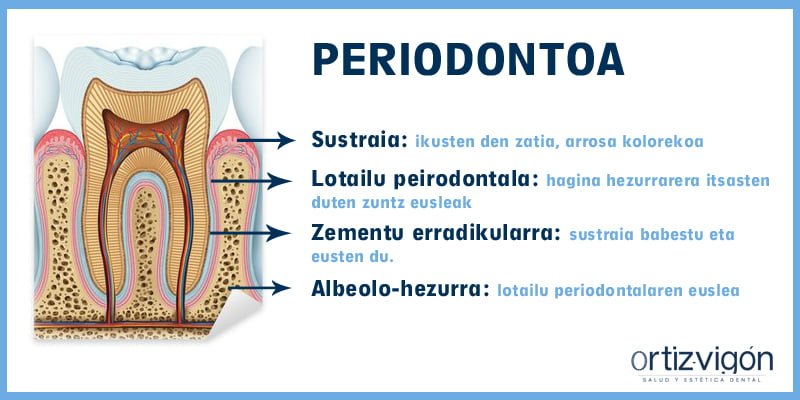
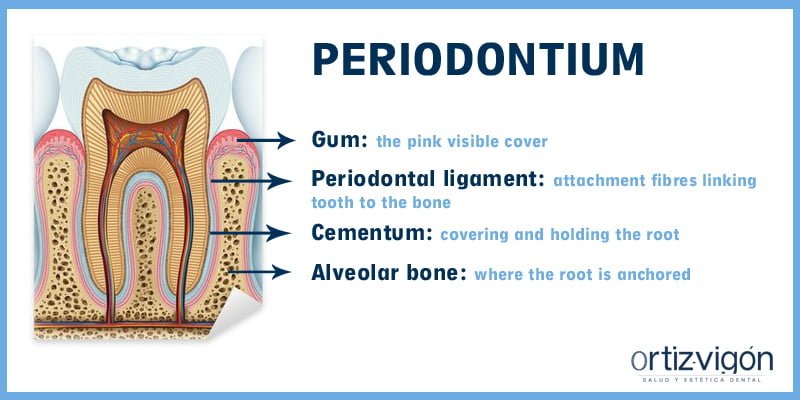
Anatómicamente el diente se puede dividir en dos partes: por un lado, está la corona, que es la parte visible y con la que mordemos; y por otro lado está la raíz, la parte no visible que sujeta el diente al hueso. Y, ¿qué es el periodonto? Son aquellos tejidos que rodean y soportan el diente. El periodonto se divide en cuatro partes:
- Encía: la parte visible, de color rosado.
- Ligamento periodontal: fibras de sujeción que fijan el diente al hueso.
- Cemento radicular: cubre y sujeta la raíz.
- Hueso alveolar: donde está anclado el ligamento periodontal.
¿Qué es la enfermedad periodontal?
La enfermedad periodontal (o enfermedad de las encías) es una enfermedad genética, que se desarrolla primero originando una inflamación de las encías secundaria a la acumulación de placa bacteriana y que, si progresa, afectará a los tejidos de soporte, provocando su destrucción.
¿A qué enfermedades se pueden asociar las enfermedades periodontales?
Las enfermedades periodontales están estrechamente relacionadas con serias enfermedades crónicas como:
- Diabetes: como ya hemos explicado en anteriores ocasiones, la diabetes y la enfermedad periodontal están estrechamente ligadas. En Clínica Ortiz-Vigón estamos desarrollando un estudio para la detección precoz de la diabetes en clínicas dentales, promovido por SEPA. ¿Cómo participar? Es fácil.
- Enfermedad cerebrovascular: que trae como consecuencia procesos isquémicos (de falta de sangre) o hemorrágicos (derrames) en el cerebro. La hipertensión arterial (HTA) es el principal factor de riesgo de la enfermedad cerebrovascular.
- Enfermedad pulmonar obstructiva crónica (EPOC): trastorno pulmonar que se caracteriza por la existencia de una obstrucción de las vías aéreas generalmente progresiva e irreversible.
- Enfermedades del corazón.
- Enfermedad renal crónica.
- Artritis reumatoidea: es una forma de artritis que causa dolor, inflamación, rigidez y pérdida de la función de las articulaciones.
Progresión de la enfermedad periodontal: gingivitis y periodontitis
En primera fase, la enfermedad periodontal se manifiesta como gingivitis, inflamación y sangrado de las encías sin pérdida de encía o hueso. La periodontitis es la progresión de la gingivitis no tratada, cuando además de la inflamación gingival, hay destrucción de la encía y del hueso de soporte.
1. Gingivitis
La gingivitis es la inflamación de las encías y puede aparecer por varios factores:
- Mala higiene bucodental.
- Procesos hormonales en el embarazo.
- Por otras enfermedades (Diabetes y otras enfermedades sistémicas).
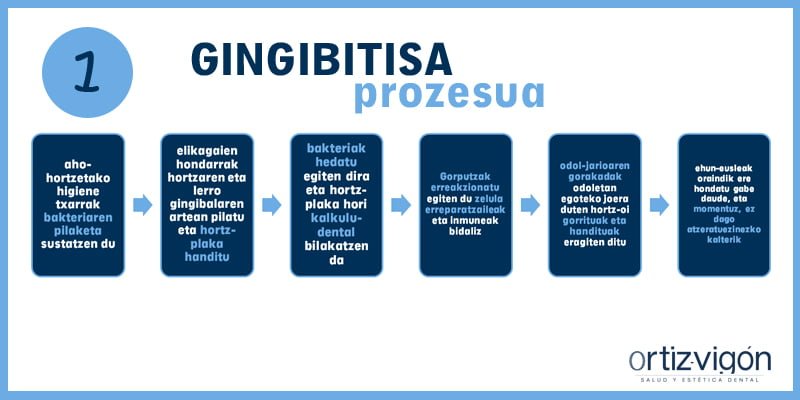
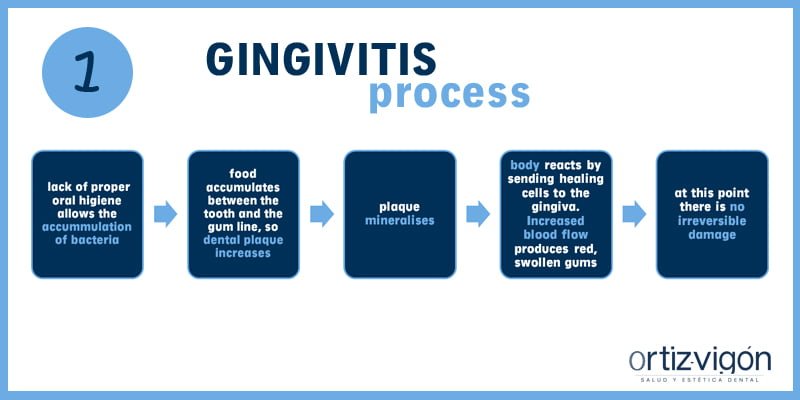
El desarrollo de la gingivitis ocurre cuando una mala higiene bucodental permite la acumulación de bacteria. Los restos alimenticios se acumulan entre el diente y la línea gingival (o línea de la encía), incrementando así la placa dental. Las bacterias se proliferan y la placa se mineraliza convirtiéndose en cálculo dental (el vulgarmente conocido como sarro). El cuerpo reacciona enviando células reparadoras e inmunes a la encía. Este aumento del flujo sanguíneo produce encías enrojecidas e inflamadas con tendencias al sangrado. En este punto, las fibras de sujeción permanecen todavía intactas y no hay, por el momento, un daño irreversible.
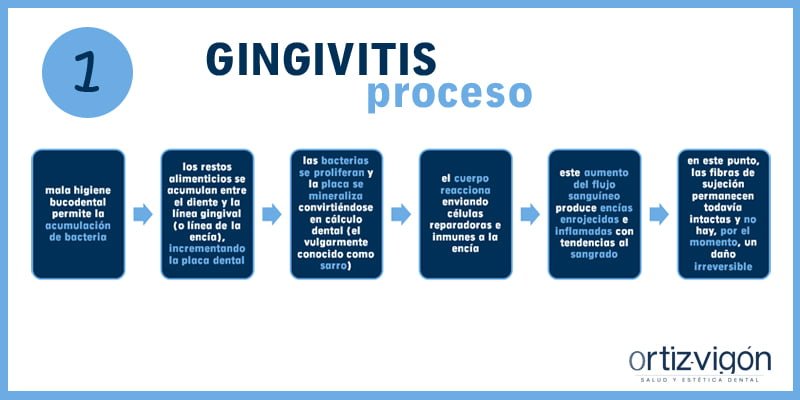
La solución para la gingivitis es proceder a la eliminación de la placa por parte de un profesional de la odontología y seguir las pautas de higiene oral que nos índice especialista en periodoncia.
2. Periodontitis
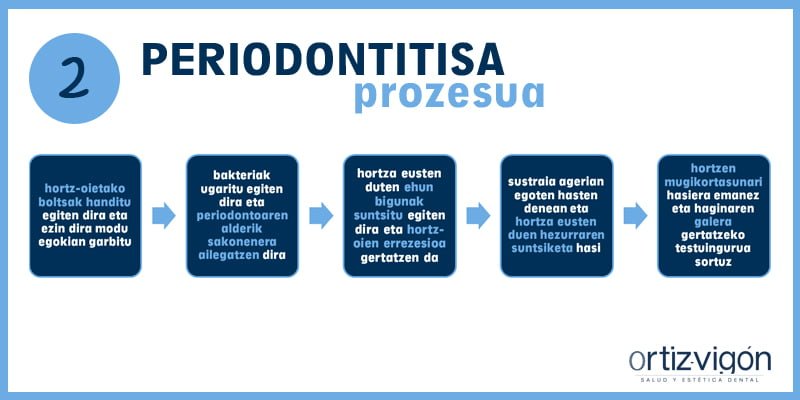
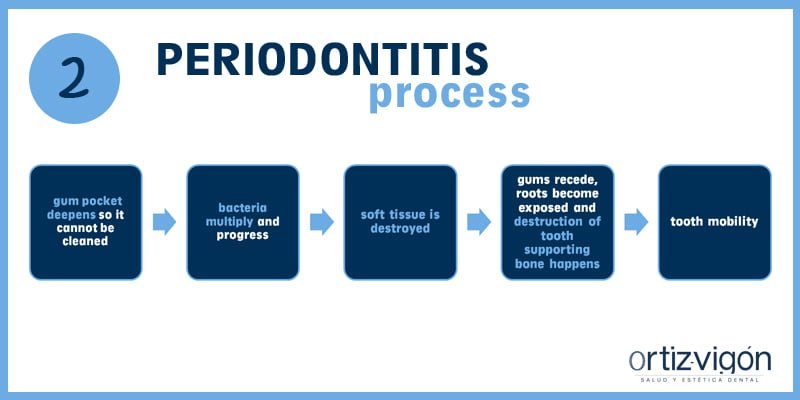
Si la gingivitis no se trata, puede desembocar en una periodontitis. Si el paciente tiene periodontitis, las bolsas de la encía aumentan y no puede llegar a limpiarse correctamente. Las bacterias se multiplican y progresan hacia la profundidad del periodonto. Los tejidos blandos que soportan el diente se destruyen y se produce la recesión de las encías. Es entonces cuando la raíz comienza a estar expuesta y empieza la destrucción del hueso que soporta el diente, dando lugar a la movilidad de los dientes y su posible pérdida.
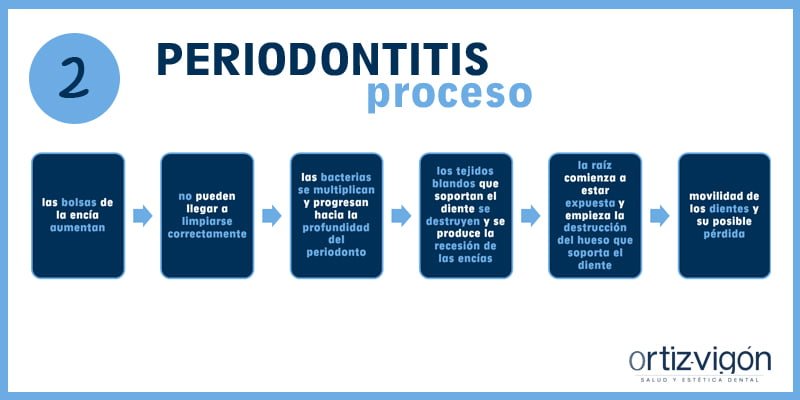
El tratamiento para la periodontitis es realizar una terapia de desinfección mediante la eliminación de la placa en la superficie radicular (en la raíz), así como una mejora en los hábitos de higiene y un seguimiento periódico por parte del periodoncista, el dentista especializado en periodoncia.
3. Periodontitis severa
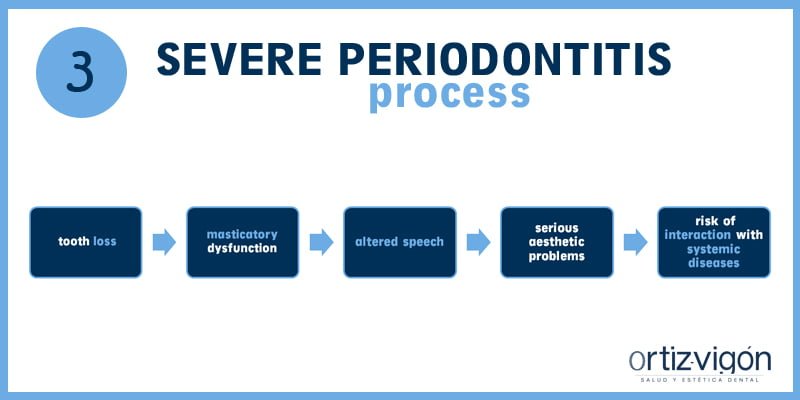
Y, ¿qué ocurre si no se trata la periodontitis? Que desemboca en una periodontitis severa. En esta fase de la enfermedad periodontal, se produce una pérdida patológica del diente, disfunción masticatoria, alteraciones en el habla, cambios estéticos importantes a medida que los contornos faciales como las mejillas se hunden y sobre todo, riesgo de potenciar y/o interactuar con otras enfermedades sistémicas (Diabetes, enfermedades cardiovasculares y respiratorias).
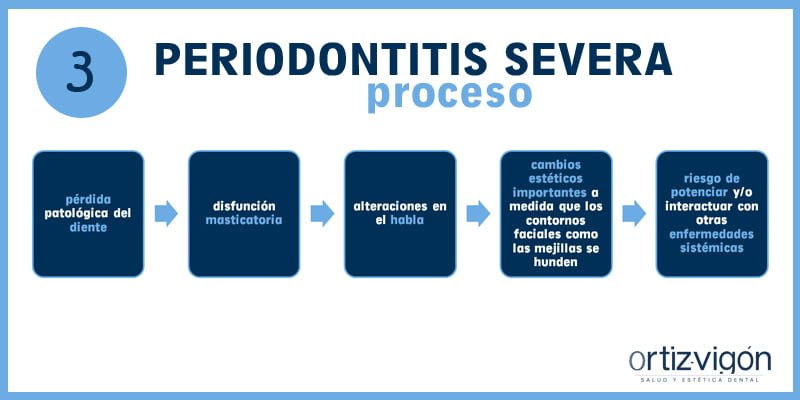
El tratamiento para la periodontitis severa consiste en una terapia de desinfección y limpieza de la superficie radicular, posible aplicación de antimicrobianos locales o sistémicos, reevaluación posterior del periodoncista y, siendo muy frecuente la necesidad de cirugía periodontal.
¿Cómo detectar la enfermedad periodontal?
Los síntomas más claros que el paciente puede detectar por sí mismo son la inflamación, el enrojecimiento y el sangrado de las encías además del desplazamiento de los dientes y el posible incremento de su movilidad. El odontólogo, detecta la enfermedad periodontal al llevar a cabo una exploración con sondaje periodontal y análisis radiográfico.
¿Cómo prevenirla?
La susceptibilidad a padecer la enfermedad depende de cada individuo. Sin embargo, sí se puede prevenir su desarrollo mediante una buena higiene bucodental, evitando hábitos como el tabaco y acudiendo a las revisiones con el especialista en periodoncia.




me gustaría saber en que consiste una obturación simple
Hola Olga,
Una obturación simple es un procedimiento en el que se restaura una pieza dental, proceso que vulgarmente se denomina “empaste”. La obturación se puede llevar a cabo por diversos motivos: porque la pieza dental tiene una caries, porque la pieza dental está rota, o bien porque la pieza dental ha sufrido una abrasión (desgaste) causada por diferentes motivos.
Para cualquier duda a nivel particular, no dudes en ponerte en contacto con nosotros/as llamando al 944 158 902.
Un saludo.
Paciente de sexo femenino de 35 años de edad acude a la consulta manifestando dolor a la masticación, sangrado gingival abundante provocado por el cepillado, aumento de volumen gingival, y movilidad dentaria generalizada, el examen periodontal revelo inflamación gingival difusa generalizada severa, al examen intraoral no se observa placa dental, perdida de NIC hasta de 8 mm. cual seria el diagnostico y tratamiento. gracias